Hi All,
It’s good to be back writing. It has been a little over a year since my last post due to life just simply being busy. This is in some ways a good thing because the whole point of going through treatments is to live life to the fullest. I recently received a message checking in on me noting that my last post wasn’t great news. I completely forgot that was my last post after not writing for so long. I’m so sorry about that! I want to update you on where things are at because there has been some great news, but also a few obstacles.
HEAD
My last post talked about how the Vorasidenib treatments were not preventing growth of an area of enhancement. Due to this, I switched over to Lomuustine and Procarbazine on February 25th, 2025. I was on these two chemotherapies for about five months when we unfortunately realized that they were not stopping growth of the enhancement. I felt pretty defeated because this was yet another treatment option taken off the shelf.
The next step was to see what other treatments were available. We looked at my past molecular report for mutations we had not targeted yet. One of the mutations was BRAF. On July 15th, 2026, I started Dabrafenib and Trametinib, which are targeted therapies for BRAF V600E mutations. We weren’t sure if this would have an effect because while my tumor has the BRAF mutation, it is a different subtype than V600E. Regardless, we gave it a try.
At my next MRI on September 9th, the MRI report read:
“Postsurgical changes of prior left frontal mass resection with slightly decreased enhancement in the resection cavity as well as slight decrease in the separate enhancing left periventricular nodule.“
DECREASE: I had never seen that word on my MRI report. Other than surgeries and radiation, none of my treatments in my 20+ years living with this has ever decreased the size of my tumor! We found the mutation that is one of the primary drivers of the tumor growth.
(right side is an older scan, left side is a recent scan. The white area just to the right of the midline is the tumor)
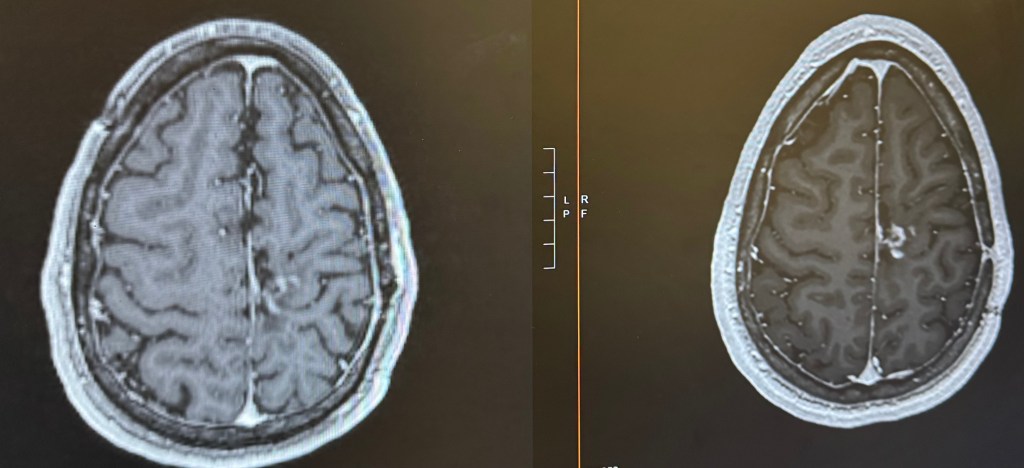
It was truly hard to believe. In the past, I would be immediately hesitant to fully accept the good news because experience has conditioned me to expect the other shoe to drop. However, one of the many things my partner, Chris, has taught me is to lean into the good news. So, I celebrated!
The next scan showed slightly further decrease in size, and my most recent scan showed stability if not further decrease. I have my next scan this Tuesday (March 17th), which I hope continues the good news. Leading up to the MRIs, I will always get scanxiety about when this ends up being too good to be true, but in between those scans I continue planning to live life fully.
HEART
Now let’s discuss another organ that seems to feel a little left out with all the attention my brain has been getting.
I was born with an abnormal aortic valve that was believed to be bicuspid – a congenital heart defect where my valve only has two leaflets when it is meant to have three.
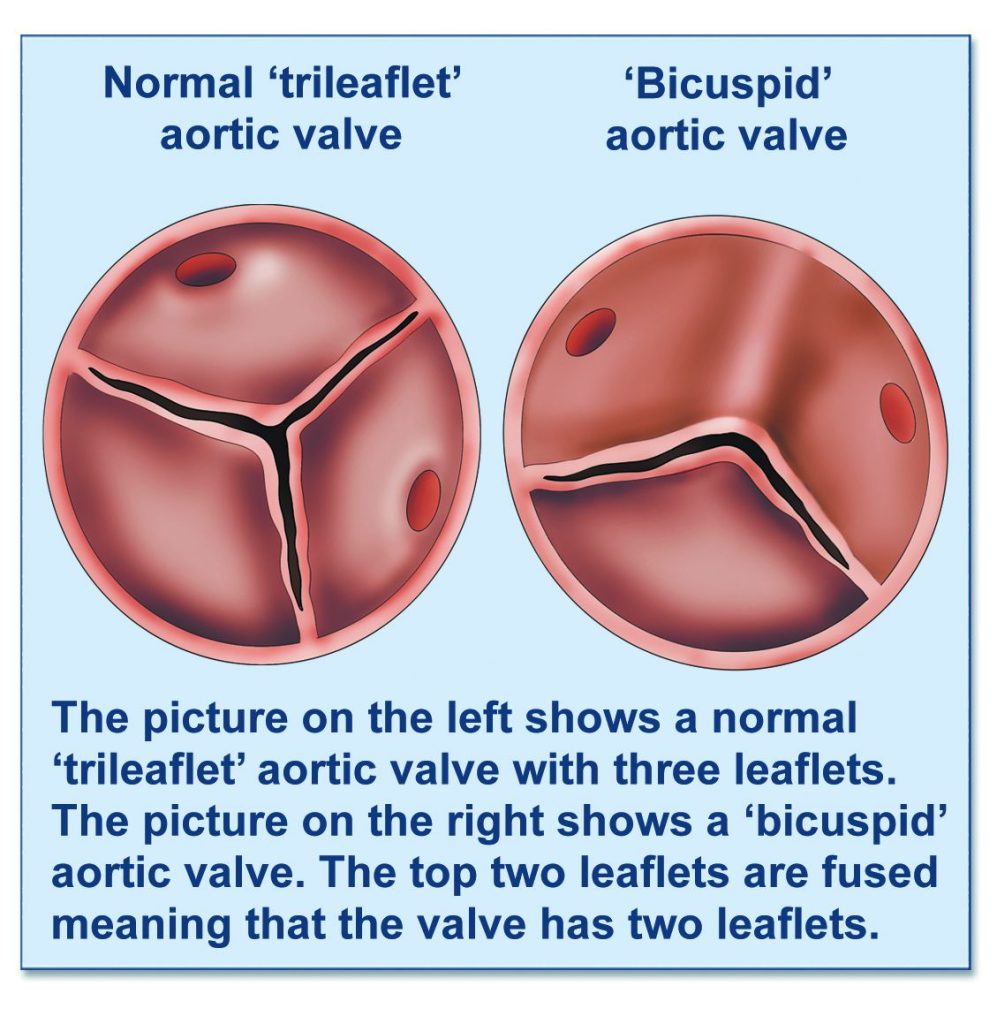
Every two or three years I would get an echocardiogram to monitor the valve. They were specifically monitoring what is called aortic stenosis, which is when the valve narrows and doesn’t open fully. This reduces or blocks blood flow from the heart to the aorta and to the rest of the body. For most of my life my stenosis has been mild. The cardiologists I had over time assumed we wouldn’t have to do anything about it until I was in my 50s or 60s.
Over the past few years, the stenosis progressed from mild to moderate. Within the past 8 or 9 months, the stenosis progressed rapidly to moderate/severe. This was not at all due to my cancer treatments, but rather some bad luck where stenosis that is usually gradual ended up turning exponential. Even though it reached the severe range, there wasn’t a need to immediately address it since I was asymptomatic. That changed this past September.
While working out, I became short of breath and could not recover for upwards of 15 minutes. While this was primarily attributed to a vasovagal reaction (i.e. not fully my stenosis), my doctors still wanted me to do a stress test.
At my stress test, I was doing really well pedaling the bike as they increased resistance. However, towards the end of the test, my blood pressure bottomed out and I became significantly dizzy. This was the first true sign of my stenosis becoming symptomatic. Additionally, I increasingly had episodes where I felt more out of breath with activities than I normally would. For example, while playing pickleball, I started feeling dizzy and out of breath just 5 to 10 minutes in, whereas just this past summer, I could play for an hour. It was time to look into what options I had available to me.
The only way to treat valve disease is to repair or replace the valve, but for my case, it is a bit more complicated. For young adults, the standard of care is a mechanical valve. However, that requires being on blood thinners for the rest of your life, which I cannot do because of my brain tumor. So, we explored what could be a less invasive procedure called the TAVR, which has a durability of 10 to 12 years until something else needs to be done.
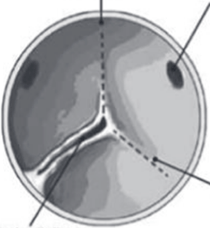
Before making any decisions, I ended up getting a CT scan of the heart in order to better see my heart and valve structure. This revealed that my valve is actually unicuspid rather than bicuspid. This means that all of the leaflets are fused, leaving just one opening:
And in addition to my valve, I also have dilation of my aorta (below is the CT rendering of my actual aorta…pretty cool to see!):
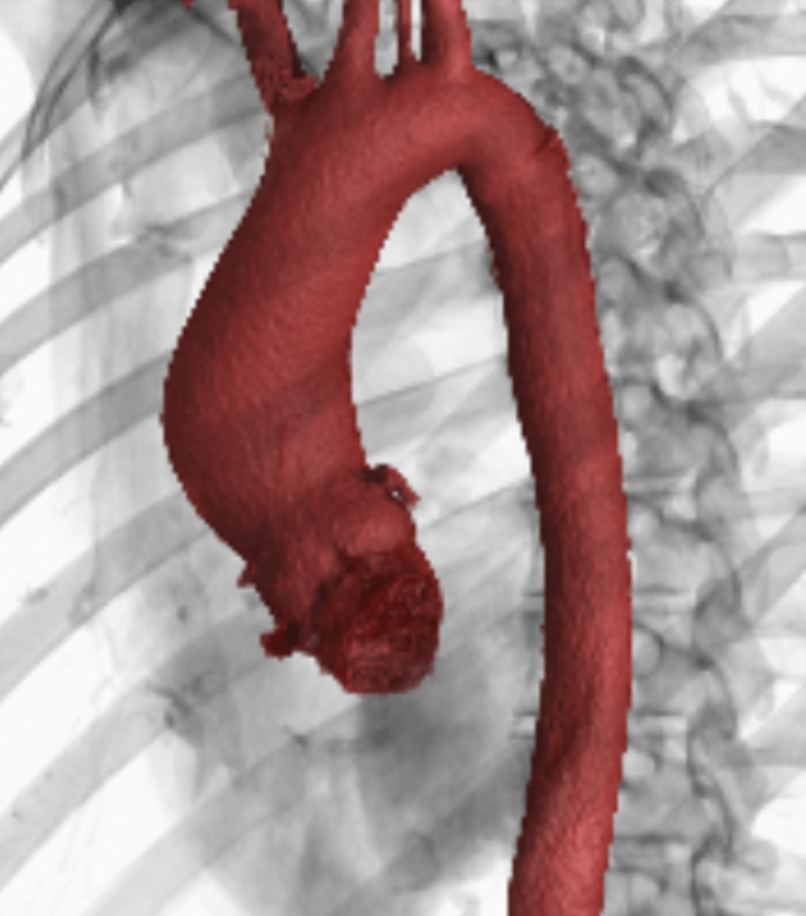
The fact that my valve is unicuspid took the less invasive TAVR procedure off the table. This left me with two options: the Ross procedure (longer durability, comparable to normal heart lifespan, but more complex surgery) or a valve replacement with a pig or cow valve (less complex surgery, shorter durability of 10-12 years). Given the difference in durability, I decided to explore the Ross procedure, and go to one of the leading Ross specialists in the country at MGH.
So what is the Ross procedure? It involves removing my aortic valve, moving my existing pulmonary valve to be my new aortic valve, and putting in a new pulmonary valve from a human donor. Pretty crazy, but given my medical geekiness, I find it fascinating. Here is a diagram to visualize it:
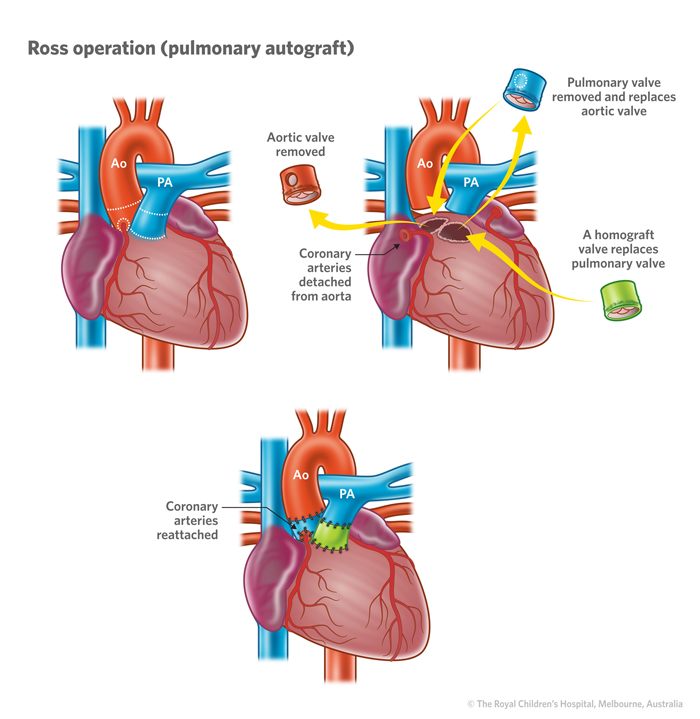
This procedure essentially makes your heart like new and is the most durable option. However, it is a highly specialized surgery. In 2023 (the last data point on record), there were 531 procedures performed in the United States. There are only about 10 surgeons in the country who highly specialize in the Ross procedure. This is important because data shows that outcomes significantly improve for surgeons who do the procedure greater than 10 times a year. Last year, my surgeon at MGH performed around 50 Ross procedures. In addition to his expertise, he is incredibly personable, thoughtful, and communicates the complexities clearly. He spent over an hour with Chris, my mom, and I answering all the questions we had. When I had further questions after a second opinion, I sent him a message on the patient portal. Usually physicians will simply reply in an email. Instead, he called me to make sure we addressed all of my questions and concerns. I feel confident that I am in good hands.
My surgery is scheduled for March 24th.
After scheduling the surgery, I initially was putting on a brave face for myself and others . It wasn’t until a few weeks ago when I broke down while with Chris that I was honest with how nervous I am feeling. One of the things that my mind is getting stuck on is the aspect of starting and restarting the heart. My brain knows that they do this all the time, but my heart (pun intended) is still latching on to this aspect of the surgery. Additionally, after the surgery, I will be taken slightly off sedation while still intubated for them to check that I can function well before they take the tube out. I was told at my pre-op appointment that this is the most uncomfortable part of the surgery (which seems pretty obvious since I am asleep for the rest of it). I’m pretty nervous about this, but I know that again, it is done all the time.
Recovery will in total be about three months with the most extensive period being the first four to six weeks. During the first month to protect my sternum I am not allowed to drive. I also need to sit in the backseat, so I am planning on getting Chris a chauffeur’s outfit :-).
My friend, Rachael, has generously put together a meal train. One of the other best ways to help is to be a “walking buddy.” I will need to walk five times a day, which can easily get monotonous. For those who are nearby, I would love company. For those who are far, I would love to virtually go on a walk together over FaceTime, or simply chat on the phone.
I think part of my emotions I talked about before are also the fact that this has all happened so soon after receiving the news about my tumor size decreasing. I thought the “other shoe to drop” would be eventual tumor progression. I didn’t think my heart would feel left out and lead me to where I’m at now.
The good news is that after this repair, I will have a heart functioning better than it has my entire life. Who knows, I might do an iron man afterwards! In all seriousness though, I’m simply looking forward to being able to be active without worrying about whether or not I will get dizzy or lose my breath. Most importantly, one month after my recovery, I will get to fully enjoy the day Chris and I get married with lots and lots of dancing.
With love,
Jeremy

HI Jeremy,
One would think that one major illness would be the limit for any one person BUT with my reproductive history I gave up on the belief that life is balanced. Bad things happen, PERIOD. I am sorry you are also dealing with heart anomalies. I know you are getting the very best of care, and your support system in your wonderful family is remarkable. I will be praying for you and sending lots of positive thoughts your way.
Best wishes,
Robin Traquina
LikeLike
Jeremy, You are an amazing man who will conquer this and any other obstacle put in your path. I would be honored to virtually walk with you when you are ready…I think of you so often and share your strength with those who need a boost. You are always in my prayers. You have an incredible support system, and I hear Chris’ positivity that will remain a source of strength for you as well🤍❤️
Love and hugs, Judie
LikeLike
hi jeremy
so great to hear from you many congratulations on your upcoming marriage!!! and i love the word “decrease” my brother had an aortic valve replaced in january…and now in cardiac rehab and doing well…and you will as well (he is much older than you!)
happy to connect again in your recovery period…would love to find a time to chat and catch up alex and lucy send their regards as well
sharada is now my co-course director for the healers art
oh, be sure to take your stone with you when you go to surgery…your surgeon will understand and then we will all be with you.
love, janet
LikeLike