Note: Before I begin this post (…again at an hour in the middle of the morning), I want to mention that all my medical results, doctor’s recommendations, and treatment decisions are my own personal experience. Each individual’s medical journey is unique. What I write is not an endorsement or recommendation for what anyone else should do. Rather, this blog serves as a window for my community, you, or someone you may know to get a glimpse into my experience living with brain cancer. Hopefully there are parts of my story that resonate, areas of connection particularly in the emotional aspects of cancer, that may be helpful to you. If you ever have questions related to what I write, please contact me.
If you are reading this post please consider donating to, or even join, Team Jeremy at the Bay Area Brain Tumor Walk on Sunday, June 24th. All funds go towards finding new treatments, and hopefully one day, a cure. My story below serves as one of thousands of examples about why this is so important!
On Monday, June 4th I had my neurooncology appointment at UCSF. Since being discharged from the hospital, my days have been pretty smooth: waking up, exercising a little, hitting an energy-wall, and relaxing. I mean how often do you get an excuse to binge-watch Netflix guilt free? As Monday approached though, I could feel the anxiety creeping throughout my body. It was the day I’d receive my biopsy results from the surgery.
We arrived at UCSF early, which was definitely a sign I was anxious because I am notoriously late for pretty much everything. I sat down with the nurse to get my vitals taken and review a list of symptoms I’ve felt in the past 30 days. While I appreciated the thoroughness, it felt never-ending…ticking off most of the boxes yes because…well…I just had brain surgery two weeks ago!
My Mom, Mark, and I finally were brought in to see the doctor. Sitting on the desk to my left was a closed, thick manila envelope. I glanced at it and thought of the exciting times in my life when I’ve received an envelope that size (…getting into college, receiving the Luce Scholarship, getting accepted to medical schools). This time was different. I didn’t want a lot of papers in that folder. The more papers, the more information. The more information, the more there is to say about the biopsy.
Surgical Results:
While my focus was on the envelope, my doctor began with showing us an MRI of the surgical results:
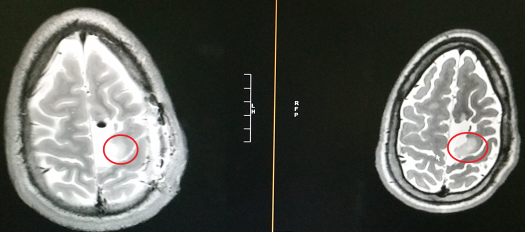
The right scan is from before my operation and the left scan is post-surgery. The large white core is the resection cavity from my surgery in 2004. Circled in red is tumor. While there are other tumor spots not shown in this scan, they have remained stable over time. What has been growing, and where our focus for treatment has been, is the area circled in red. You can see in the image on the left that they were able to remove a lot of the tumor (about 40%) up to the point where the tumor is located within the motor cortex that controls critical motor function for my right side (particularly my arm, hand, and wrist). The remaining tumor is inoperable.
Biopsy Results:
My doctor opened the envelope and pulled out the first page. It read:
- Biopsy 1: Grade III Anaplastic Oligodendroglioma
- Biopsy 2: Grade III Anaplastic Oligodendroglioma
- Biopsy 3: Grade III Anaplastic Oligodendroglioma
My doctor continued talking, but like putting on noise-canceling headphones, all the sound in the room muffled. I felt my chest tighten, tears welling up, but used the energy I had to keep myself composed and listen to what my doctor had to say.
In retrospect, I wish I gave myself permission to cry at that moment. I wish I paused the conversation and felt the raw emotions welling up inside. The biopsy results were the worst case scenario, and I should have been okay to feel that sadness. Feel the turmoil, twist and turns, of this roller-coaster that began 6 months ago with my seizure on Christmas Eve.
Since I was twelve years old I’ve lived with a low-grade (grade II) Oligodendroglioma. While I had been living with brain cancer for 14 years, I found myself lucky that my tumor was slow-growing and thus more like a chronic illness than anything incredibly imperative at the moment. Unfortunately, as this type of tumor sometimes does, it evolved to the most aggressive form it can be (…very rarely can an oligodendroglioma transform to the most aggressive type of brain tumor, a glioblastoma).
My doctor started talking about UCSF’s treatment recommendations. I usually turn into patient-mode and take copious notes on the computer. Yet while I had my computer in hand, I couldn’t get myself to write. I had a recording going, so knowing I could listen back on the conversation, I sat there and talked for almost an hour and a half with my doctor.
In reality, only part of me was present in that conversation. The rest of me was somewhere else, drifting, trying to process what these results mean for my “new normal.” I’ve lived with brain cancer practically my entire life. I’ve understood my reality of living with illness, the constant uncertainty it entails. Grappling with living life in the face of never-ending uncertainty has led me to live fully, striving to embrace the present each and every day. It’s shaped the person I’ve become, the types of relationships I foster, as well as the experiences and opportunities I’ve sought. I built a boat, with the help of family and friends, and knew how to navigate this ocean of a low-grade glioma.
Now, with these biopsy results, I didn’t know how to navigate these new seas. I still don’t. Can I use the same boat? Do I need a different boat? (…I prefer sailboats, so hopefully that can suffice). What’s this new normal mean both for my present and future? I still don’t fully know, and given my life-history with this tumor, its location, and it’s unique pathological and molecular makeup, I’m an N of 1. Meaning, there is no past research group I fit into that can tell my doctors and I what this means for my life and what treatment is best. There is no standard of care.
If I were to go to five different medical institutions, they would likely give five different treatment recommendations. As my doctor at UCSF put it, at this point treatment is based on Gestalt, or to put it in English rather than Yiddish, the art of medicine. This art is why doctors can never be replaced by Google. Despite all the information available, all the research done, at some point these decisions come down to the doctor’s intuition, based on the most up to date knowledge, expertise, and prior experience. To observe doctor’s practice their art for the betterment of their patients is one of my favorite parts of medical school.
Just like there are various forms of art, there are different opinions on how to treat what I have. UCSF has one opinion and my doctors in Boston have another. I will be heading back to Boston next week to meet with my doctor there, and will write more about treatment options then.
On that Monday what I soon realized after hearing the differences in treatment opinions is that it is more important for me to choose an artist, not the art. I am beyond privileged that I have access to the best artists there are, the best doctors available for the cancer I have. There is not one artist that is better than another, there is just the artist I prefer…my favorite artist…and that is my neurooncologist at Dana Farber. He’s the one I’ve developed a relationship with since my recurrence in 2014. He’s the one who understands my values the best. He’s the one who knows how to communicate with me and I with him. He’s the one I trust. I chose my surgeon based on my gut, and all I can do at this point is choose my neurooncologist in the same way. To be able to do that is a privilege few people have. It is one I do not underestimate, and it is why I plan to do all that I can to get through this and create value from my experience to help and give back to others.
Brunch
After receiving all this news, my Mom, Mark, and I went to brunch because…why the hell not? There are some things that are out of my control, but there are plenty of things I still can control. I can still go out and have a dam good delicious brunch.
We treated ourselves and went to Zazie, one of the best spots in the city and close to UCSF. Its now become our bad-news brunch go-to locale. The last time we were there was when I found out about this whole new saga of a recurrence months ago. Thus, it seemed fitting to commemorate this new bad news with what is some of the best eggs, potatoes, and pancakes in town.
I joke a bit about something this serious because in the end what’s the point if you can’t find some humor, if you can’t take time to have a good meal with the people you love.
In some ways these biopsy results change everything and nothing. I don’t have a full grasp on what this new reality looks like, but I don’t see how this changes my values and how I’ve learned to live in the face of life’s fragility. Yes, the uncertainty may be amplified, the stakes may be higher, but if anything, that is even more of a reason to continue to live fully in the present. This will be easier said than done, but I plan to take a hopeful, realistic mindset with these new cards I’ve been dealt.
Hope for treatments…Hope for a cure
I can be hopeful, but there are also actions I, you, and others can take to foster hope. I am not alone in what I’m facing. I’m not the only N of 1 who is needing to rely on the art of medicine rather than evidence-based established treatments or cures for brain tumors. Despite an estimated 700,000 Americans living with a brain tumor, there have only been four (yes 4!) FDA approved drugs – and one device – to treat brain tumors in the past 30 years. These drugs have provided only incremental improvements to patient survival with mortality rates remaining little changed in the past 30 years. I find this unacceptable.
But there is hope. As a medical student, I’ve had access to seeing the plethora of treatments coming down the research pipeline. With the advent of genetic testing there has been ground-breaking work in understanding the genetic drivers of brain tumors and thus avenues for targeted therapies. Even in the few years since my recurrence in 2014, there have been major gains in clinical trials and treatment development. In fact, in a couple weeks I should receive the results of my tumor’s genetic testing which may help reveal alternative treatment options.
There is no new research, there are no new treatments, and there will be no cure if there is no funding. So if you did make it to the end of my post, please again consider donating to, or better yet, fundraising for Team Jeremy at this month’s Bay Area Brain Tumor Walk. Every dollar counts, every dollar gives a little bit more hope to me, but more importantly, it gives hope for all those in the future who may have to face this illness. If the privilege I’ve had in my experience, if my fundraising, advocacy, and writing can help others in need, then it will all be worth it.
With Love,
Jeremy

Dear Jeremy,
Thank you for sharing the progress of your journey. You are remarkable to both being with the illness and outside it!! Remarkable insights about the challenging life situation. I wish you well and most importantly, to live well.
as a cancer survivor, I find that finding MEANING of LIFE the most important and challenging task of this life situation.
In my case, spirituality has been of help.
Take care and prayers for the best outcome for you.
The following quote from Marilyn French, about the perception of time and living in the present has been helpful.
“I no longer have large scale desires. I no longer wish for or expect undying love, perfect harmony within my family, a life in which everything is right (which, however absurd it may be, I did desire and kept anticipating before). I have only small desires- for a glass of cold orange juice, a good book, a visit with someone I love. Not only do I have no large desires for myself; I no longer have them for the world. Coming up against the absolute limit of death destroyed my fervent belief that an ideal world would be created if only people would do X and Y, believe what is before their eyes, let themselves be happier. It destroyed my absurd and unconscious belief that because I could see the ideal, I had the responsibility to help others see it, to create it. The weight of this responsibility was heavy, and carrying it made me angry. I was also angry because I was frustrated that no matter how simple it all was, it was not happening@.
“Coming close to death as I did engraved on my consciousness the understanding that the ideal is not going to happen, that it was always a delusion, the daydream of a wilful child, engraved upon my body by yearning and misery and helplessness like the faulty tattooed on one’s body by acid-dropping needles that prick it as the sinner is turned around and around on a huge rotisserie, in Kafka’s The Penal Colony. Coming up against failure in so absolute a fashion calmed my anger and cooled my ambition. I am no longer driven, I no longer imagine I can do much to help bring about the millennium of the human ideal, or that I can change anything at all. I have relinquished my painful freight. I am free. I am permitted to enjoy myself. I have noticed that my laugh has changed, is more spontaneous, deeper. I am almost serene. I can not say that I am happy that I was sick, but that I am happy that sickness, if it had to happen, brought me to where I am now. It is better place than I have been before. I am grateful to have been allowed to live long enough to experience it.”
Srinivasa Murthy
LikeLiked by 1 person